Updated October 27, 2023.
Everything you need to know about fodmaps.
What are FODMAPs?
It is an acronym, each letter represents a family of ingredients which can cause problems. In fact, it’s all about carbohydrates, sugars, which are poorly digested and ferment in our intestines.
- F for fermentable, it is not a family, but it is to introduce the fact that all the following carbohydrates can ferment in your intestines.
- O for oligosaccharides (fructans and galacto-oligosaccharides, or GOS)
- D for disaccharides (lactose!)
- M for monosaccharides (ingredients containing too much fructose)
- A for « And »
- P for Polyols (sorbitol, mannitol, xylitol, maltitol…)
Why follow a (low) fodmap diet?
Note that the diet does not cure irritable bowel syndrome, it only prevents its digestive disorders.
This diet was initially developed for people suffering from Irritable Bowel Syndrome (IBS) and has been shown to be highly effective in reducing the disorder (about 75% success, source 1 and 2).
But other patients are increasingly being redirected to the low-fodmap diet: those suffering from endometriosis, fibromyalgia, SIBO (bacterial overgrowth of the small intestine) and chronic inflammatory bowel diseases such as Crohn’s disease or ulcerative colitis, which can often combine IBS in addition to these diseases.
Concretely, the diet consists in avoiding certain foods known to cause disorders. If we want to be more precise, we must speak of a diet low in fodmaps, because the aim is not to exclude them entirely, far from it.
Foodmap or fodmap?
It’s fodmap, one “o”. Nothing to do with “food”, since fodmap is the acronym explained above.
The fodmap diet for weight loss?
No!
Despite its name, the fodmap “diet” is by no means a diet designed to lose weight.
Yes, it makes the “belly flat”, but not because you lose weight, simply because you don’t swell! I’ve seen people whose belly went from “flat” to “6 months pregnant” in two or three hours because of the fermentation from high-fodmap ingredients.
🤰
Why it’s important to get a solid diagnosis
If you have not been diagnosed with IBS, then there is no point in following this diet, in fact it is strongly discouraged.
Don’t self-diagnose! If you suspect you have one of these diseases: do yourself a big favor by going to see a gastroenterologist. It’s quite fast and very simple.
Why the fodmap diet is scientifically proven and solid
It started in 1999 with Sue Shepherd and Peter Gibson, two Australian scientists. Their university, Monash University (Melbourne), is the absolute reference in this field worldwide. Here I explain the scientific approach taken to establish the fodmap diet and to assess the robustness of the studies (the dedicated article will be there soon).
There you go, you can send this article to the skeptics who look up when you tell them you’re on this diet and tell them it’s not a trend or your latest fad.

Silvia Trigo’s picture on Unsplash.
How do we determine the fodmap levels in food?
That’s right, how do you get that level of accuracy? Who puts out these numbers? How is it measured? I’m explaining all this here.
Temporary or permanent diet?
There is a lot of confusion about this.
No, you don’t have to eat “fodmap-free” for life. Only during phase 1 which lasts between two and six weeks (see next section).
However, once you reach the 3rd stage, the fodmap restrictions are for life. Discover the three steps to fully understand the subtleties.
The fodmap diet in 3 steps
Step 0: preparation
The first step requires great rigor. For a few weeks, if you don’t follow the instructions to the letter, the whole test may be distorted and you may wrongly conclude that this diet doesn’t work for you.
All it takes is one deviation for your stomach to suffer for two, three or four days (a meal in a restaurant with colleagues, a chocolate bar at break time, a piece of chewing gum…).
You have to completely change your habits. Banning certain ingredients, weighing everything, checking any composition in restaurants or when you go shopping, stopping almost all industrial food and much more home cooking on your own, planning your lunches for your workplace or university, knowing what to replace certain things with, how to avoid products such as milk, wheat or onions, etc.
Step 1: exclusion
Also known as the “eviction” phase.
Basically, we start with a phase of avoidance where any ingredient high in fodmaps is left out. This phase lasts 4-6 weeks and should see a clear improvement in symptoms. If this works, it means that this diet is suitable for you, you can then move on to phase 2.
Even though it usually takes a month, you can start to see the benefits in just a few days (less than a week), however some people only see the benefits after three weeks to a month, so don’t get discouraged and stay vigilant about what you eat.
You should therefore avoid ingredients that are rich in FODMAPs, but personally I find that this term, although it makes scientific sense and is easy to remember, is not the most practical.
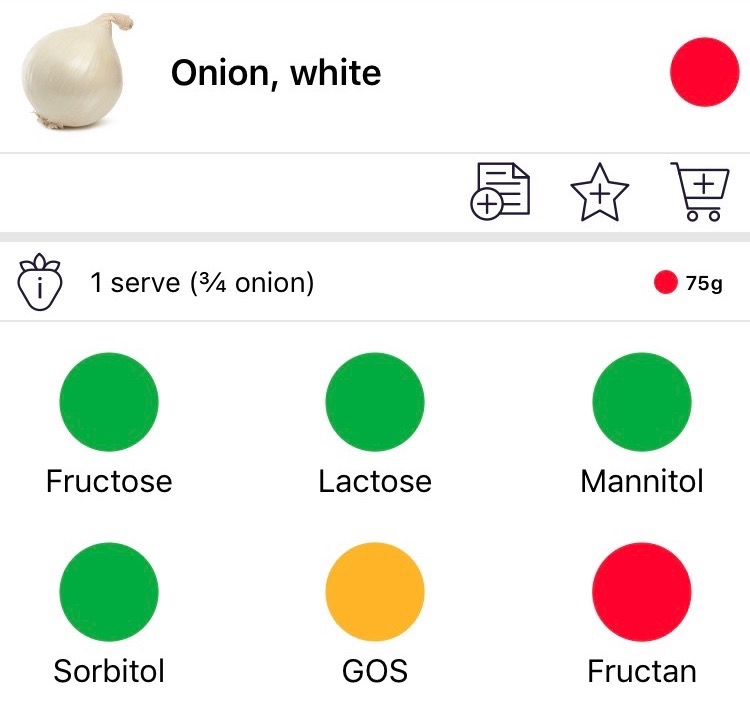
In practice, that is not what we are going to look at. The “F” and the “A” are not families of ingredients, and within the “O” and the “P” there are several families. So what I’m going to look at instead is this list of six:
- lactose
- fructans
- GOS (galacto-oligosaccharides)
- fructose
- sorbitol
- mannitol
Write down what you eat in a food diary
Keeping a food journal of everything you eat is essential and extremely useful. Whether you’re just starting out or have already started the fodmaps method, it’s never too late.
Find all the interests of keeping a journal and my free-to-download template here.
Step 2: reintroductions
The reintroduction phase consists of testing each of the families (fructans, lactose, fructose…). There is a good chance that you are not intolerant to all these families: by testing them one by one, you will be able to find out.
This process takes weeks and is not easy to carry out. For some families the answer will be very clear (no problem = complete reintroduction; or large reactions, big trouble caused = avoidance), but for others it may be less clear, leaving you in doubt.
The risk is to remain in a phase of perpetual eviction, which is discouraged because it is dangerous and will lead to deficiencies, isolation and may lead to the development of eating disorders. This phase 1 should absolutely not be maintained over the long term.
It is essential to be trained (buying books, reading articles or watching videos from reliable and up-to-date sources) and being accompanied by a professional such as a dietician is an undeniable bonus that can shorten the duration and complexity of this phase.
Step 3: customization and cruising speed
You know what you can tolerate, what you can’t and in what quantities.
You will then:
- Fully reintroduce food of families that do not trigger any symptoms,
- Reintroduce in limited quantities foods in families that cause you moderate disorders,
- Banish those which cause you significant disturbance.

Photo from Tanner Yould sur Unsplash.
No fodmap diet VS low-fodmap diet
The difference is huge. As mentioned above, leading a diet without fodmaps over time can lead to nutritional deficiencies, to avoiding your friends, family and professional circle and can even lead to more or less serious eating disorders.
You should not go on a diet without fodmaps, or just a few weeks during the eviction phase and again this is not recommended, you can eat some “normal” bread or milk even during this phase. It’s all a question of quantity, which requires weighing everything and a great deal of rigor to organize yourself.
I know, it’s hard. That’s why it’s essential to remain informed, to get involved, it takes time, and why not get professional help.
Why are fodmap lists contradictory?
If you search on the internet, you will certainly find contradictory lists. This is a real problem that we have all faced.
Why? Some people make mistakes, the subject is complex, but above all because research has evolved and brought about subtleties. See this article for more details on contradictory lists.
It is imperative that you refer to a reliable and recent list (maximum 2 years).
A life process to check again later
Even if today there is no solution to cure irritable bowel and this diet is therefore for life, this does not mean that there are no change to be expected.
Our gut microbiota is a living organism that is very sensitive and constantly evolving. It is not impossible that your fructose or lactose intolerance may be less severe or even disappear entirely in a few months or years.
That is why it is recommended to re-test from time to time, with the goal of perhaps reintroducing more foods. This can greatly facilitate your daily life, your social life, when you are at a restaurant, with friends, family or when you go shopping. Or maybe to cook one of the recipes again that you used to love but had to give up.
Limits and criticism of the fodmap diet
This diet is not a fad or a lifestyle choice, it is a constraint for those who follow it and responds to a real medical condition (Irritable Bowel Syndrome).
Step 1 (exclusion), although complex but due to its relatively short duration (6-8 weeks maximum, more often 3-4 weeks), shows very good success rates.
The main criticism of this diet is its practical implementation regarding Step 2 and 3. In fact, many people may get “lost” and do not complete this 3-step method [Source 3]. One of the risks is to remain on a “fodmap-free” diet (see above), to remain stuck in step 1.
Fodmapedia
I have IBS myself and I created the tools I wish I had. I’ll be delighted if they will help you:
- The fodmapedia.com database, with foods adapted to our diet,
- This blog,
- The newsletter:
Get your old life back
Get rid of your Irritable Bowel problems by succeeding with your FODMAP diet, thanks to the most comprehensive FODMAP food database, Fodmapedia.
Fodmap sources used for this article
- [Source 1] Does a diet low in FODMAPs reduce symptoms associated with functional gastrointestinal disorders? A comprehensive systematic review and meta-analysis, 2016 research paper.
- [Source 2] The low FODMAP diet improves gastrointestinal symptoms in patients with irritable bowel syndrome: a prospective study, research paper from 2013.
- [Source 3] Controversies and Recent Developments of the Low-FODMAP Diet, 2017 research paper written by Peta Hill, Jane G. Muir and Peter R. Gibson of the Monash University.


Combinations. Are they discussed anywhere?
For example, are modest quantities of two things problematic? Is their specific type important to consider? (eg, fructose and manitol)
Thanks!
Very good question. I’m actually getting ready an article about this exact topic, but yes, modest quantities of two things could be problematic. I’m warning you as soon as it’s published.
There you are, my article about FODMAP stacking! https://blog.fodmapedia.com/en/stacking-fodmaps/